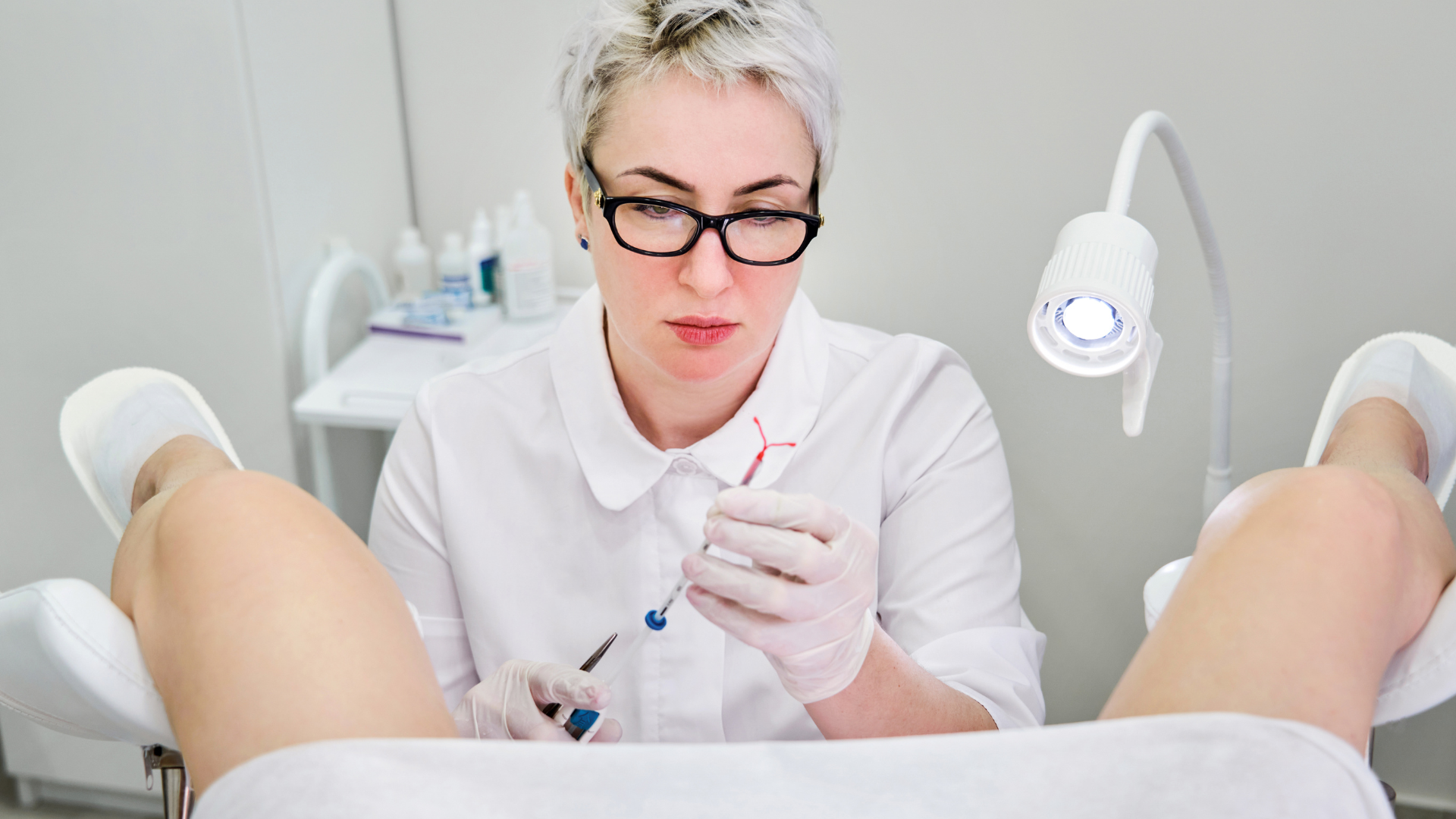
IUD insertions are routine, in-office procedures that, including consultation and prep and getting dressed again after, take only about 10 minutes.

Acquiring your IUD
Presumably the process and experience varies by country and by doctor, but this how it went for me, in Canada:
In Canada, most extended (group) health insurance covers the IUD prescription. In my case, that’s 90% coverage so the approximately $400 Mirena IUD is only about $40 for me, and is approved for 7 years. Prices will vary depending on where you are, so if you’re interested in getting one, ask your doctor about the least cost prohibitive options in your area and look into accessible resources like Planned Parenthood or your local equivalent.
Once you have your prescription for your IUD, any pharmacy can fulfil the prescription usually within a day or two. You will need to bring your IUD, in original packaging, to your insertion appointment. Do not open it before hand.
Standard Procedure, Stirrups and All
The appointment is much like a PAP smear. You’ll be asked to undress from the waist down and “assume the position” on the exam table. The IUD can be inserted during your period and you can usually get one put in right after giving birth or having an abortion. If you’re not on your period you can request to have a PAP done while they’re down there. If there is any chance you may be pregnant, your doctor will do a pregnancy test as well (which will require you to give a urine sample).
The doctor then inserts a speculum in the vagina to hold it open and expose the cervix. Before insertion, the doctor will swab your cervix with iodine to disinfect the area and prevent infection. They’ll then push in a graduated rod to measure the depth of your uterus. This helps them position the IUD properly.
“You’re Going to Feel a Little Pinch …”
The IUD is inserted by way of a long, thin plunger that pushes the little T-shaped device through the muscular ring of the cervix. The top crossbar of the T-shape is flexible and the arms bend back and pop out again once it’s in place.
The only substantial pain I experienced in the whole procedure was the actual insertion. When the IUD pushes through the cervix, it causes your uterus to cramp. Yes, it hurts. However, for me, the pain was momentary and like a bad menstrual cramp. It is not standard to freeze or numb the cervix before the insertion. You are welcome to ask for a topical analgesic to numb it and take the pain down a notch. If you wish to have an injection for freezing, talk to your doctor about that before your appointment.
Strings Attached
The strings are trimmed so that a centimetre or two protrudes from the cervix and remains in the vagina. The strings enable your doctor to remove the IUD when it’s time for a new one. This also allows you to check that the IUD has not become dislodged. Check every month or so by squatting and feeling for the strings with your fingers. If you’re concerned that your IUD has moved, see your doctor.
Feeling lightheaded, sweaty or nauseous for a few moments after the insertion is totally normal. Take your time sitting up if you feel woozy. Ask your doctor for a sip of water or juice if you feel faint.
Pain
As mentioned, and this is only MY experience: the pain incurred from an IUD insertion was very, very brief. There was a sharp pinch, some pressure, and then it was over. As soon as it was in, the pain went from an 8 to a dull 3. Pain is very subjective so I won’t say it was nothing, but I found it very manageable and was over very quickly.
IUD Insertion Recovery
Some lingering discomfort and cramping is normal and usually subsides within a few days to a week. Avoid lifting anything heavy or having penetrative vaginal sex for a few days if you are tender. Ibuprofen or whatever you usually take for menstrual cramps should be enough to manage any pain or discomfort. If you have off the charts pain, talk to your doctor/gyno, or go to Urgent Care.
You may have some spotting in the days after the insertion. The iodine will flush out of your vagina and cause oddly brown looking discharge the first day – do not be alarmed. If you are unsure about how you feel or what to expect, contact your doctor or a nurses’ helpline.
The IUD lessens or eliminates periods for many people and within a month or so your body will have regulated. In my case, my period disappeared within my first cycle and stayed away for over 5 years. Everyone’s body is unique though, so give yourself some time to adjust.
Your doctor may ask you to come back into the office to review any concerns. They can also recommend options if you decide that the IUD is not for you. If there were issues with the insertion or other complications, an ultrasound may be necessary.
My Second IUD
I have had great luck with the IUD and it eliminated my heavy periods and solved anaemia. My red blood cell count is normal and I no longer require iron supplements.
Research says that the incidence of pregnancy in the 6th and 7th years of having an IUD only increases by less than 2%. Because I have such medical anxiety, I pushed the limits on the lifespan of my IUD and mitigated conception risks with condoms (even with fluid-bonded partners) once my regular period re-surfaced.
My gyno let me know that because I waited past the expiration date and the hormone dose rapidly diminishes, I might have more bleeding in the first 2 months with the new IUD than I did with the first one. This is because the lower dose of hormones allow the uterine lining to re-establish itself, hence the regularly timed periods. Ultimately, this was not the case and I have not had a single period or breakthrough bleeding in the 3.5 years since I had the second IUD placed.
What You Need to Know If You Are Considering an IUD
IUDs come in several brands, and 2 distinct styles. There’s hormonal release IUD (like Mirena) and the copper coil IUD (like Paragard). Do your research and work with your doctor to decide which IUD is best for you.

Like any birth control method, IUDs are not infallible. They have a very low failure rate of >1% when inserted correctly and used as the primary form of contraception.
IUDs do not prevent against STIs. They can increase the instance of Pelvic Inflammatory Disease if inserted when the patient has an existing STI. Talk to your doctor about your STI history so that she can recommend alternatives if the IUD isn’t appropriate.
If you’re non-monogamous an IUD is just fine for pregnancy prevention. But if you are still using barrier methods (condoms, dams, etc) regarding STI risks, those risks are not diminished by an IUD. Play safe!
Side Effects and Benefits
I have experienced zero negative side effects beyond the usual discomfort during recovery each time I had the IUD inserted. I use the Mirena (the highest dose hormonal IUD available and most likely to eliminate periods). My periods are gone but I still get a couple days of (emotional) PMS each month, but no cramps or bleeding.
Loss of libido, acne, depression and weight gain have all been associated with the IUD. Different types and brands yield different results and in many cases, the long term benefits out weigh the (mostly) short term side effects.
IUDs Work Well For Me, But I Am Not You
In my case, the Mirena IUD basically saved my life. It put a cease and desist on menstruation and allowed my body to replenish its blood supply and in time I overcome the anaemia I suffered from. For me and my lifestyle, it is perfect. No periods interrupting life in general. No condoms (other than with new partners), and the threat of pregnancy is nil.
My IUD gives me confidence, both in my overall health and my sexual health. It has allowed me to feel in control of contraception while not having to buy, prepare, remember, or use contraception in the heat of the moment. I am really happy with my choice to get a second one.
I Enthusiastically Recommend the IUD
… if you are a good candidate for it. It is worth researching and discussing with your doctor. Making fully informed decisions regarding our bodies and health can be overwhelming but it’s an important to try our best.
You deserve care and medical services without stigma. Take it from me, someone who in their 40s still cries from fear and stress every time I have to go to a doctor’s office: You can do it. Research, ask questions, and advocate for yourself. Then make decisions that work for you and your body because you know it best.
Have you experienced an IUD? Share your wisdom in the comments below!

